When Liam Dee and Jacob MacDonald swore marriage vows to one another, fewer than 20 people were in the room. COVID-19 restrictions still loomed over the March 2022 ceremony in Wolfville, Nova Scotia, and since they’d moved up the wedding date several times, there were a lot of last-minute snafus in the chapel.
Realizing they hadn’t picked a song to walk down the aisle to, the couple asked for the classic one everyone uses—not thinking about how a track titled “Here Comes the Bride” might be a misnomer for two men. In the middle of the ceremony, they suddenly remembered they’d left the rings in the car.
Yet the hiccups added to the relaxed charm of the intimate ceremony. “It was such a perfect day,” says MacDonald.
The road to their wedding was winding. The two met in Fredericton, New Brunswick, when MacDonald was in his senior year of high school and Dee, a forestry student at the nearby college, still identified as straight. On their first date in 2016, MacDonald recalls how Dee couldn’t shake his nerves. “Liam was pretty awkward at the time—he was on a bit of a self-discovery journey.”
Dee went on to have a girlfriend, but the two men stayed connected. Despite the rocky start, Dee’s mother—Cindy Gates-Dee—says that after Dee did come out, he still thought about his initial spark with MacDonald. “He was like, ‘Mom, I met this guy, I really, really like him, but I was so weird—I don’t think I’m ever going to see him again.’”
But they did reconnect in 2018, and this time Dee was ready. Now openly gay and back at school to become a nurse, he had a greater sense of self. They’d bond over their mutual rural upbringings on Canada’s East Coast. Their shared love of nature translated into dates hiking the nearby Crystal Falls. Dee talked about his hobbies, which MacDonald would come to learn were extensive. “He’d always be picking up something new, teaching himself something. I felt inspired by his drive.”
The two got serious and made plans for the future. After graduating early, Dee moved back in with his parents in late 2021 to save for a home the two of them could buy in the province’s scenic Annapolis Valley. They dreamed of a summer wedding.
But shortly after making this move, a pain in Dee’s shoulder—which he’d experienced on and off for years—became more pronounced and prolonged. Concerned, his mother brought him to her doctor, initially thinking it was arthritis. After running some tests, the results were grim. Despite being young and otherwise healthy, Dee learned the source of his suffering was likely cancerous. They moved the wedding up five months.
Dee’s official diagnosis came just nine days before the wedding: liposarcoma, a rare and life-threatening cancer that had formed a large tumour in his chest. While the prognosis was bleak, the couple remained determined to enjoy their special day. “Our mindset was, well, you’re here right now. We were able to put that out of our mind and just really be in the moment.”
“Dee’s official diagnosis came just nine days before the wedding.”
After the wedding, things precipitated quickly. Instead of buying a home together, MacDonald moved in with Dee and his parents and shared caregiving duties. In just months, Dee transitioned into hospice. After exhausting all treatments—including removing his left lung—he passed away on Nov. 10, 2022, at age 26.
Through their grief, Dee’s loved ones knew he had gifts to share in death just as in life. The cancer meant his organs were too damaged to donate, but arrangements were made to donate Dee’s tissues—including skin, corneas, tendons and bones—to others in need.
These were Dee’s wishes both in hospice and years before, when he signed up as a registered donor (nearly a decade before Nova Scotia adopted an opt-out donation policy in 2021). The hospice staff obliged, contacting the Nova Scotia authority responsible for facilitating such a donation—yet no collection would take place.
“As soon as they found out from the hospice nurse that Liam had a husband, that shut the conversation down immediately,” says MacDonald. He and Dee’s mother pushed for more information. After all, everyone at the hospice believed that Dee would be able to donate.
Dee’s mother had to hound the donation bank for more information on why Dee’s donation was rejected. When Dee’s family finally did get to review the paperwork, they learned his donation was rejected due to “high-risk sexual behaviour,” despite no one asking Dee or his long-term, monogamous partner any questions about their sexual lives or history.
“It felt like being slapped in the face,” says Gates-Dee, still in mourning from losing her son, and now shocked that this type of discrimination could still be happening.
Dee’s case isn’t unique. Queer men (and trans women) across Canada and globally are being denied or flagged as donors. While we don’t have reliable numbers on exactly how many total donations are rejected for this reason, one study found that when it came to corneas alone—a tissue donation that can return someone’s sight—as many as 3,217 donations by otherwise eligible queer and trans donors in the U.S. and Canada were rejected in 2018.
These rejections are based on policies stemming from the 1980s, when the HIV/AIDS epidemic was at its height and queer men were contracting the virus at dizzying rates. HIV could, after all, be passed on via blood, tissue and organ donations. “Since then, though, the landscape around HIV detection, prevention and treatment has changed completely,” says Dr. Murdoch Leeies, an organ donation specialist and researcher at the University of Manitoba.
Leeies explains that since the ’80s, we’ve created better and more reliable HIV tests—able to detect the virus’s presence within smaller and smaller “risk windows” (the time between infection and when tests would reveal positive results). What was once six months became three, and is now as few as 10 days.
There are also new ways of preventing and treating HIV. PrEP and PEP are highly effective medications to prevent HIV transmission. Antiretroviral therapy can help someone achieve what’s called “undetectable” status, rendering their viral loads so low that they are unable to pass on the virus (also known as U=U, or undetectable equals untransmittable).
So while there is a risk that donations fall within the “risk window” for standard testing—not yet revealed as positive for HIV—there are so many other factors to consider, like if a donor is on PrEP or has achieved U=U.
“To say men who have sex with men is a risk factor for HIV is a broad overgeneralization,” says Leeies.
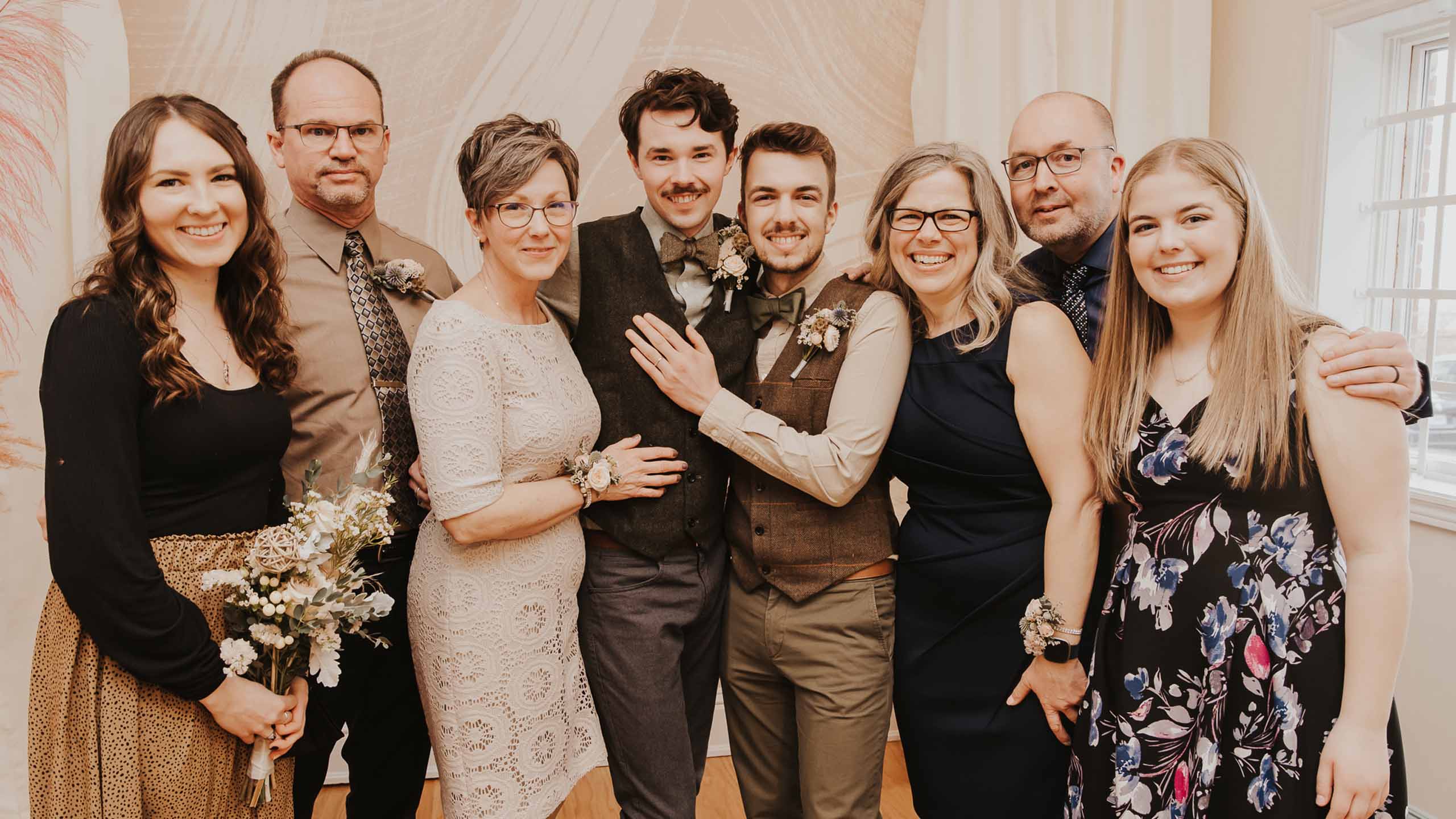
A photo of Liam Dee (left) and Jacob MacDonald and their immediate families at their wedding ceremony Credit: Courtesy of Jacob MacDonald
The chasm between the latest scientific understanding of HIV and policies around medical donations has been a point of contention for years—especially when it comes to the much more common practice of donating blood. Queer men and trans women were also once banned for life from donating blood in Canada and the U.S. due to HIV risk.
However, after years of advocacy from the queer and trans community, the rules around donating blood have changed. In Canada, that lifetime blood donation ban was whittled down and down until 2022, when Health Canada adopted a gender-neutral, behaviour-based questionnaire for all donors. The U.S. Food and Drug Administration (FDA) followed suit earlier this year.
If a similar policy was adopted for other medical donations, Dee’s final gift would have been accepted—but the same change in approach has yet to hit organ and tissue policies, in part because of the overlapping and intertwined network behind such donations.
“If a similar policy was adopted for other medical donations, Dee’s final gift would have been accepted.”
For instance, U.S. organ donation is regulated by the Health Resources and Services Administration, whereas tissue donation is overseen by the FDA. In Canada, rules are set by the federally run Health Canada, but processed through provincial organ and tissue donation agencies that are accredited through the U.S.—meaning that unlike blood donations, organ and tissue donations go by American regulations, which are much more restrictive than Canada’s.
This means that even if Health Canada adopts less restrictive donation policies for queer men and trans women, provincial bodies are likely to still flag organs and tissues as “high-risk” based on U.S. rules—which right now say that if you’re a man who has had sex with another man in the past five years, your donation will be rejected.
Leeies explains that’s likely why Dee’s hospice care team believed him to be able to donate his tissues, despite ultimately being rejected by the Canadian donation agency. “Canadians are being exposed to the regulations of a foreign nation.”
When asked about why Canadian donation agencies follow American guidelines, a spokesperson for Health Canada told Xtra that they do create and enforce regulations around tissue and organ transplants. Even so, individual agencies still elect to follow stricter U.S. guidelines. According to the spokesperson, Health Canada has asked the Canadian Standards Association to create a working group to discuss potential changes to the donor screening criteria for men who have sex with men. This group began meeting in July 2023, but no timeline or deadline on progress was given.
But it’s a wonder why it took so long for the group to be formed. As far back as 2019, a bi-partisan committee of MPs officially recommended the government take action to make blood, organ and tissue donations less discriminatory to queer and trans people. When asked about progress on this recommendation from his colleagues, a spokesperson for Canada’s health minister, Mark Holland, deferred to Health Canada’s response to Xtra.
These policies are not only discriminatory—they also keep potential donors from contributing to a severely under-resourced pool. At the start of 2022, more than 3,700 Canadians were on wait-lists to receive an organ transplant. Last year more than 270 Canadians died while waiting. In the U.S., over 104,000 people are waiting for an organ transplant—and on average, 16 Americans die every day from the lack of available organs. It’s less clear what wait-lists are like for tissue donations, as those can often involve small-scale operations.
To demonstrate how valuable donations can be, a single organ donor can save up to eight lives and improve the lives of as many as 75 others.
As our population ages, the need for organ and tissue donations keeps increasing. Despite improvements in the tally of organ donations in Canada over the past decade, the number of people in need of a transplant has outpaced that growth.
Because organs are so desperately needed and life-saving, a recipient can elect to still receive a “high-risk” donation in what’s called “exceptional distribution.” That’s what happened with the heart, liver and kidneys of Joseph Keenan. When the Pawtucket, Rhode Island, hairdresser passed away in 2018, his husband, Billy Partain, was glad to see that three lives were saved thanks to exceptional distribution.
But there is no such recourse for tissues, despite the potential quality of life improvements they can offer recipients, such as the aforementioned corneas offering someone their eyesight back or bone donations preventing the need for amputation. As such, Keenan’s tissues were rejected outright even though he had been in a 20-year long monogamous relationship. That fact still frustrates Partain today.
“It was so hard for me to process that you could take his organs, which are made up of tissues, but you wouldn’t take anything else,” Partain says. “I still can’t make any sense of it and it angers me.”
Despite the incoherent policy, Partain is glad his husband was able to donate his organs. “It was a silver lining in my tremendous loss,” he says, recalling having brought a stethoscope to his first encounter with the person who received his partner’s heart. “Being able to hear my husband’s heart again gave me so much peace. It helped in my healing.”
Even now, years after his husband’s donation, Partain remains close to Keenan’s heart recipient and considers them part of his family. He still joins them at events, usually with a stethoscope in hand. They’ve become so close that the recipient’s grandson’s middle name is Joe, for Keenan.
When Partain heard about Dee’s story through donation advocacy circles, he mourned for Dee’s husband and mother—knowing they would not experience the same comfort in having a piece of your loved one live on.
“If Liam would have been able to donate his corneas and give the gift of sight to someone, I know that that would have helped in their grieving and healing. Being denied that is just so heartbreaking.”
It’s a heartbreak that Gates-Dee feels deeply. “His skin could have helped a burn victim. His tendons could have helped someone potentially walk again. That angers me.”
When Partain asked the recipient of Keenan’s heart why he accepted a high-risk donation from a gay man, the recipient said it was a no-brainer. He had gay friends, he didn’t buy into the HIV stigma and—most important—he wanted to live.
That’s a sentiment shared by many others, says Brandon Bayton—a Washington, D.C.-based communications professional and donor advocate. “There are so many people out here who just don’t care what sexuality you are. What they want to do is live.”
As a gay man and recipient of two liver transplants, Bayton knows that fear can cloud a recipient’s judgment. On his first transplant, he rejected high-risk donations. But when it was time for his second, he understood the process and science around HIV better, and opted to accept high-risk donations, including from queer men.
Bayton worries that these discriminatory policies feed into that fear, making potential recipients reject exceptional distribution donations from otherwise healthy gay men—not to mention doing “a great disservice” to the already small and in-demand donor pool. Though the number of voluntary organ rejections isn’t reported, studies have found that passing on an available donation increases the risk of the recipient dying or getting so sick they’re no longer a candidate for transplant.
And since many people don’t know about exceptional distribution, stories about rejected tissue and high-risk organ donations reinforce the idea that queer donors are not welcomed, which can deter would-be donors. “There’s a large percentage of queer people who just don’t believe that they can donate,” says Bayton. “We need outreach and education for the community.”
Now that blood donation policies, though still flawed, are less overtly exclusive of queer men, an increasing number of community advocates are turning their attention to organ and tissue policies. Bayton and Leeies are both part of efforts to gain political traction around this issue, with the latter authoring a report with the Canadian queer health-focused Community-Based Research Centre.
The report makes the case for donation policies more in line with our latest understanding of HIV, as well as calls to end practices that expose or dehumanize queer bodies. One such practice includes a physical rectal exam of a corpse to find “evidence” of receptive anal sex—suggesting that they may be a high-risk donor. This is done at the discretion of the doctor, but recommended by the Canadian Standards Association for all deceased male donors.
“That test does not have a scientific basis to accurately predict what it’s proposing to,” says Leeies, who decries the process as being an unreliable way to tell if someone is having anal sex or has an increased risk for HIV. It also lacks consent and can retraumatize a deceased person’s loved ones, especially if they’re from a country where same-sex sexual activity is outlawed, and forced rectal exams are used to collect evidence. “It’s stigmatizing and discriminatory.”
“No other family should feel this way because their loved one has been denied.”
Leeies advises those who are upset over that practice—or any of the limitations placed on queer donors—to contact their federal representatives. Though organ and tissue donations are processed through a fractured, Americanized system, the federal government and Health Canada are best positioned to start untying those knots. They can embrace more inclusive and evidence-based policies, better regulate local actors and fund more robust training for healthcare workers in this space.
“By us blowing the horn and identifying these issues, we force the system to engage with this,” Leeies says.
But Gates-Dee is not waiting for the government to wake up and realize this is a problem. On behalf of her son, she has filed a case with the Canadian Human Rights Commission. “No other family should feel this way because their loved one has been denied.”
The case is still pending, and the family worries about the pushback they’re getting from the commission about filing a human rights complaint on behalf of someone deceased. MacDonald says that if they’re rejected on those grounds, he’ll file one himself. “They really did rob Liam of the legacy that he wanted to leave—and they robbed us of the opportunity, as a family, to have his wishes met,” says MacDonald.
This fight for equality has become Dee’s new legacy, and it’s one that bonds Gates-Dee and MacDonald—a family brought together by a man with talent, ambition, a love of learning new things and a desire to help other people.
This past June, on Dee’s first birthday since his passing, his family chose a memorial that honoured both beauty and strength. On a sunny afternoon, they gathered a group of loved ones at their home to plant a crabapple tree on their property in memory of their son. The group shared stories, told jokes and celebrated Dee’s life.
Through their pending case, Dee’s loved ones are determined to continue to honour him. “There are lots of ways that we’ve memorialized Liam, and we think about him all the time,” says MacDonald. “We’re hoping that this fight can really be his legacy.”


 Why you can trust Xtra
Why you can trust Xtra


